One in five cancer patients in Derbyshire diagnosed via emergency admission
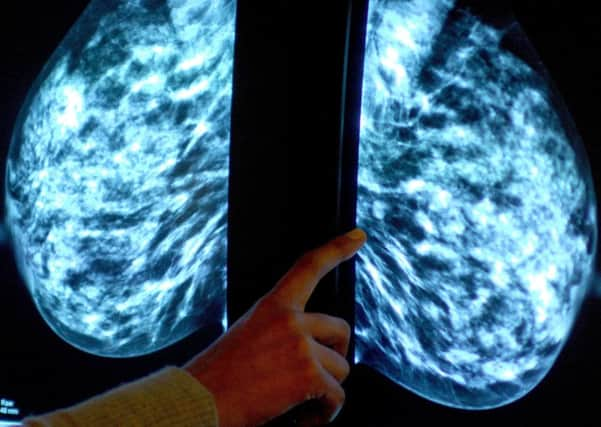

The survival rates of emergency admission are substantially worse than routine referrals as patients are more likely to have more advanced and difficult to treat cancers.
Cancer Research UK has called for more awareness, better training of GPs and increased resources for the NHS to help ensure more people are diagnosed early.
Advertisement
Hide AdAdvertisement
Hide AdIn the 12 months to March, 2,576 patients were admitted to hospital with cancer in the NHS Southern Derbyshire Clinical Commissioning Group area, according to data published by Public Health England.
Most will have been referred by their GP or other routes such as breast or cervical screening programmes.
But 497 patients - 19.3% - were classed as an ‘emergency presentation of cancer’, meaning they were first diagnosed at the hospital, after coming to A&E, for example, or while being treated for something else.
Fiona Osgun of Cancer Research UK said it was important for patients to see their GP if they noticed a change in their body.
Advertisement
Hide AdAdvertisement
Hide Ad“Your chances of survival can change so much if the cancer is diagnosed earlier or later”, she said.
“Generally, if the symptoms are severe enough to cause an emergency presentation, it is highly likely that the cancer is advanced.
“The treatments that we know give the best chance of cure like surgery are either harder to do or aren’t medically viable at stage three or four.
“So your treatment options are limited, and in some cases you’re not going to be treating the patient for a cure by that point, but treating them palliatively.”
Advertisement
Hide AdAdvertisement
Hide AdAccording to the latest annual Cancer Patient Experience Survey, 14% of cancer patients in south Derbyshire who went to their GP surgery with a cancer-related health complaint before they were diagnosed said they saw their GP three or four times before being told to go to hospital.
A further 6% had five or more appointments.
But the reasons behind emergency presentations are “complex” and not necessarily the result of symptoms being missed by GPs, Ms Ogsun said.
Some cancers, such as brain cancer, have vaguer or more sudden symptoms than others, while GPs are also reliant on the wider NHS system to investigate quickly after a referral.
She continued: “We know that endoscopy is really stretched in the NHS at the moment for instance, and we are going to see more and more pressure placed on them with an ageing population.
Advertisement
Hide AdAdvertisement
Hide Ad“We need more workers and money across the NHS. We need action on all fronts.”
In south Derbyshire the proportion of emergency cases has fallen since 2016-17, when they made up 21.6% of cancer diagnoses.
Across England, the proportion has been coming down over the last few years, dropping from 19.5% in 2016-17 to 18.8% for 2017-18.
According to the latest figures, covering April to June 2017, 50% of patients diagnosed at the NHS Southern Derbyshire CCG had stage three or four cancer.
Advertisement
Hide AdAdvertisement
Hide AdThe average across England was 48%, but ranged from a low of 37% to a high of 63% depending on the CCG.
There was also significant variation across the country for the proportion of emergency presentations, which ranged from 14% to 26%.
Dr Jem Rashbass, cancer lead at Public Health England, said: ‘‘PHE publishes the latest data on variation across the country to help commissioners and health providers better understand their cancer population and identify areas for improvement.
“PHE’s Be Clear on Cancer campaigns aim to raise awareness of the symptoms of cancer and encourage those who have symptoms to go to their GP.”